Looking for Expert-Level VA Claim Answers?📱Call Us Now! 737-295-2226
If you have been diagnosed with ischemic heart disease (IHD), it’s important to be aware of the other conditions that can occur. This guide will provide an overview of the most common conditions secondary to ischemic heart disease.
Knowing what to look for and how to manage these conditions can help you maintain your health and lead a fulfilling life.
Table of Contents
Deserve a Higher VA Rating?
Book a no-obligation VA Claim Discovery Call with an experienced team member. We’ll review your situation, spot what the VA may have missed, and help you map out a strategy to unlock the VA disability rating and tax-free compensation you’ve earned for your service. Click the red button below to book your call.
Ischemic Heart Disease
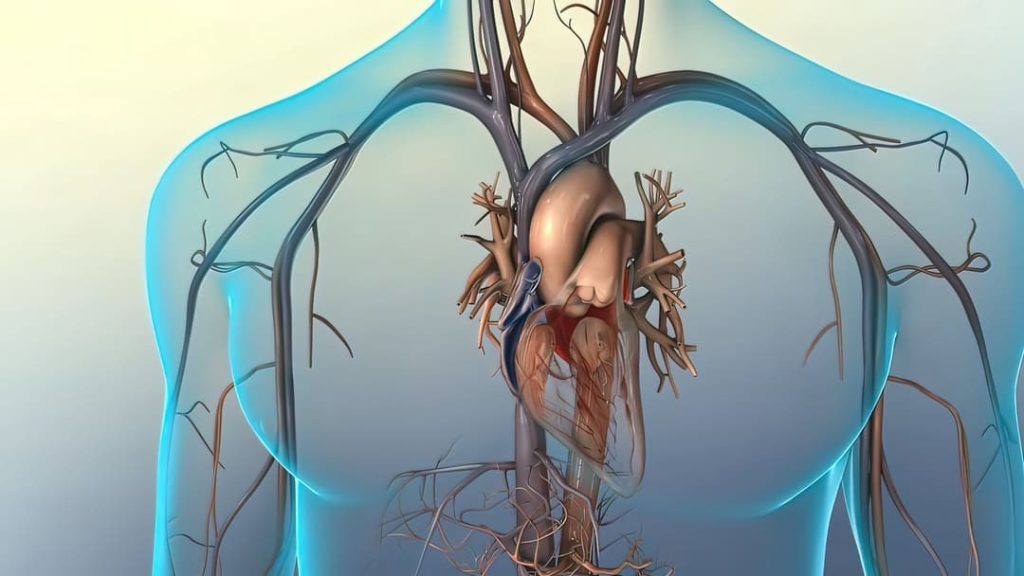
Ischemic heart disease, also known as coronary artery disease (CAD) or coronary heart disease, is a condition that occurs when an artery supplying blood to the heart muscle becomes blocked or narrowed. It can be due to plaque buildup, which is made up of fat, cholesterol, and other substances.
Over time, plaque can harden and narrow the arteries, making blood flow difficult. It can lead to chest pain, shortness of breath, and other symptoms.
Ischemic heart disease is a major cause of death among veterans. While there is no cure for the condition, you can manage it through lifestyle changes and medical treatment. A stress test is important in diagnosing and managing ischemic heart disease.
C&P Exam for Ischemic Heart Disease
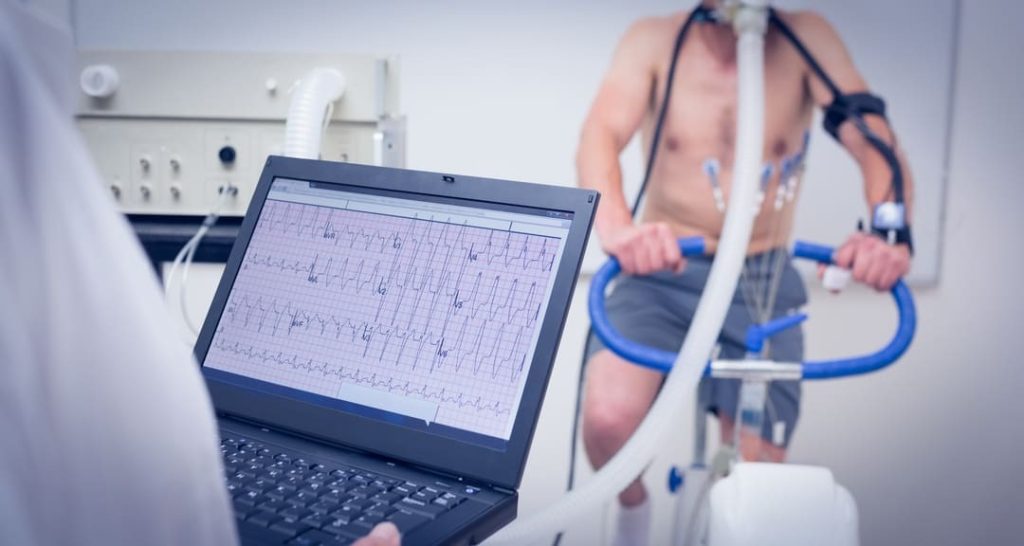
An ischemic heart exam, commonly called a “stress test,” can provide your doctor with important information about your heart health. It’s vital the physician performing your exam gets a MET (metabolic equivalent of task) test done for ANY heart condition.
The test is usually performed while you are exercising on a treadmill or stationary bike. As your heart rate and blood pressure increase, your doctor will monitor your heart’s electrical activity and blood flow.
If your heart is healthy, it can pump enough blood to meet the increased demand. However, if you have ischemic heart disease, the reduced blood flow can cause the electrical activity to become abnormal. In addition, the stress test can also help your doctor determine how well your heart is pumping and how much reserve capacity it has.
Ischemic Heart Disease and Agent Orange
Agent Orange is a herbicide used by the U.S. military during the Vietnam War. The chemical has been linked to various health problems, including cancer, congenital disabilities, and ischemic heart disease.
Several studies have shown an increased risk of ischemic heart disease among veterans exposed to Agent Orange. The exact mechanism by which the chemical causes this condition is not yet known, but it is thought that it may interfere with the normal functioning of the heart muscle or the arteries.
If you have been exposed to Agent Orange, it is important to talk to your doctor about your risk factors for ischemic heart disease.
Average Disability Payment Agent Orange Ischemic Heart Disease
Veterans exposed to Agent Orange during the Vietnam War are at an increased risk for developing ischemic heart disease, and many receive disability benefits as a result. There’s no data that shows the average VA rating for ischemic heart disease. The disability compensation depends on the disability rating.
The VA rates IHD between 10-100%. The monthly disability compensation ranges from $152.64 to more than $3,330.
VA Secondary Conditions to Ischemic Heart Disease
Several conditions can occur as a result of ischemic heart disease. These secondary conditions can significantly impact a patient’s quality of life and, in some cases, can be life-threatening.
Some of the most common secondary conditions include sleep apnea, heart failure, arrhythmias, cardiomyopathies, and valvular heart disease.
By understanding the VA secondary conditions associated with ischemic heart disease, veterans can take steps to prevent further complications and improve their overall health.
Sleep Apnea Secondary to Ischemic Heart Disease
Sleep apnea is a condition that can be caused by several factors, including ischemic heart disease.
Sleep apnea occurs when a person’s breathing is interrupted during sleep, often causing them to wake up gasping for air. It can happen multiple times throughout the night, leading to serious health problems like fatigue, high blood pressure, and heart disease.
One of the main risk factors for sleep apnea is obesity, which other conditions like ischemic heart disease can also cause. When the heart doesn’t get enough oxygen-rich blood, it can cause the muscles in the airway to relax, leading to obstruction and sleep apnea.
Related:
Ultimate Guide to Getting a Sleep Apnea VA Rating!
Massive Changes Coming to VA Ratings for Sleep Apnea!
Heart Failure Secondary to Ischemic Heart Disease
While the symptoms of heart failure can seem to come out of nowhere, the condition is often the result of another underlying cardiovascular problem. One of the most common causes of heart failure is ischemic heart disease, which occurs when the arteries that supply blood to the heart muscle become blocked or narrowed.
It can lead to a heart attack; over time, it can weaken the heart muscle and cause it to pump less efficiently, leading to fluid buildup in the lungs and other body parts, resulting in heart failure’s characteristic symptoms.
Because of this close relationship between ischemic heart disease and heart failure, it’s important for anyone diagnosed with one of these conditions to be closely monitored by a cardiologist.
Although heart failure can be filed secondary to IHD, the VA won’t assign separate ratings. If the VA grants service connection for both conditions, they will only assign whichever condition has the higher rating.
Arrhythmias Secondary to Ischemic Heart Disease
Arrhythmias are a common symptom of ischemic heart disease and can often be a sign that the condition is progressing. Arrhythmias occur when the heart muscle cannot pump blood effectively, which can cause the heart to beat too fast or too slow.
In some cases, arrhythmias can lead to cardiac arrest. In addition to being a secondary condition to ischemic heart disease, arrhythmias can also be caused by other conditions such as hypertension, diabetes, and obesity.
Treatment for arrhythmias usually focuses on addressing the underlying condition and may include medications, lifestyle changes, or surgery. In some cases, implantable cardioverter-defibrillators may be recommended to help prevent sudden cardiac death.
While arrhythmias can be serious, most people with the condition can manage their symptoms and live long, healthy lives.

Cardiomyopathies Secondary to Ischemic Heart Disease
Cardiomyopathies are a group of disorders that affect the structure and function of the heart muscle. They are a leading cause of heart failure and death worldwide and are one of the common secondary conditions in veterans with ischemic heart disease.
Cardiomyopathies can be caused by various factors, including genetic predisposition, viruses, toxins, and medications. They can also occur due to other conditions, such as diabetes, hypertension, and obesity.
Cardiomyopathies often lead to abnormalities in heart function, including arrhythmias, chamber dilation, and reduced pumping ability. The most common symptom of cardiomyopathy is shortness of breath, but patients may also experience fatigue, chest pain, and lightheadedness.
Early diagnosis and treatment are essential for managing cardiomyopathies. Treatment options include lifestyle modification, medications, implantable devices, and surgery.
Similar to other heart conditions secondary to ischemic heart disease, the VA won’t assign separate ratings. If the VA grants service connection for both conditions, they will only assign whichever has the higher rating.
Valvular Heart Disease Secondary to Ischemic Heart Disease
Heart disease is a general term used to describe various heart conditions. One type of heart disease is valvular heart disease, which occurs when one or more of the heart’s valves are damaged. It can cause blood to leak back into the heart or flow in the wrong direction.
Valvular heart disease is often a secondary condition to another form of heart disease, such as ischemic heart disease. Ischemic heart disease occurs when the arteries that supply blood to the heart muscle become blocked. It can cause a Heart Attack, the most common type of valvular heart disease.
People with ischemic heart disease are at an increased risk for developing valvular heart disease, so it is important to be aware of the symptoms and get regular checkups.
As mentioned previously, with other heart conditions, although valvular heart disease can be filed secondary to IHD, the VA will not assign separate ratings. Similar to other heart conditions secondary to ischemic heart disease, the VA won’t assign separate ratings. If the VA grants service connection for both conditions, they will only assign whichever has the higher rating.
Ischemic Heart Disease VA Rating
The VA rates ischemic heart disease under the General Rating Formula for Heart Conditions with a range from 10% to 100%.
A 100% rating is given if a MET test causes symptoms (like shortness of breath, fatigue, chest pain, dizziness, heart palpitations, arrhythmia, or fainting) at 3.0 METs or less.
A 60% rating is given if a MET test causes symptoms (like shortness of breath, fatigue, chest pain, dizziness, heart palpitations, arrhythmia, or fainting) at 3.1 to 5.0 METs.
A 30% rating is given if there is one or more of the following:
- An MET test causes symptoms (like shortness of breath, fatigue, chest pain, dizziness, heart palpitations, arrhythmia, or fainting) at 5.1 to 7.0 METs.
- Evidence (echocardiogram, multigated acquisition scan, MRI, etc.) of hypertrophy or dilatation.
A 10% rating is given if there is one or more of the following:
- An MET test causes symptoms (like shortness of breath, fatigue, chest pain, dizziness, heart palpitations, arrhythmia, or fainting) at 7.1 to 10.0 METs.
- Continuous medication is required for control
Ischemic heart disease is a serious condition, and it can have a significant impact on a veteran’s quality of life. The VA will consider the severity of the veteran’s symptoms. It will also look at any treatment received to determine the appropriate rating.
Frequently Asked Questions (FAQ)
How to Prove Service Connection
Service connection links your present disability and your active military service. To receive benefits, you must first prove that there is a service connection.
The best way to do this is by providing a complete medical history and linking it to your military service records. Your medical records should include all treatment received for your condition before and after your discharge from the military.
You can increase the chances of successfully demonstrating a service connection by completing the three parts of the Caluza triangle:
- You have a medical diagnosis of a disability condition.
- You provide evidence of an in-service event, injury, disease, or aggravation.
- You have a nexus (or link) between #1 and #2 via competent medical evidence, such as a Nexus Letter.
It can also be important to document and disclose your “Severity of Symptoms” in terms of their frequency, severity, and duration.
Is Hypertension Secondary to Ischemic Heart Disease?
Some experts believe that hypertension may contribute to ischemic heart disease, but the exact relationship between the two conditions is unclear.
Hypertension, also known as high blood pressure, is a condition in which the force of blood against artery walls is too high. It puts extra strain on the heart and can damage the arteries. Over time, hypertension can lead to coronary heart disease, heart failure, stroke, and kidney failure. While it is often possible to control hypertension through lifestyle changes and medication, some people with hypertension also develop ischemic heart disease, which occurs when the arteries that supply blood to the heart muscle become blocked or narrowed.
What Are the Different VA Heart Condition Ratings?
Veterans who develop heart conditions due to military service may be entitled to disability benefits from the Department of Veterans Affairs (VA). The VA assigns a disability rating to each condition based on the severity of the condition and its effects on the veteran’s ability to work and live a normal life. The following are the different ratings that can be assigned to heart conditions:
All heart conditions are rated on the General Rating Formula unless otherwise noted. The General Rating Formula for heart conditions ranges from 10% to 100%, with breaks at 10%, 30%, 60% and 100%.
Related: VA Disability for Heart Conditions
Does Sleep Apnea Cause Coronary Artery Disease?
There is growing evidence that sleep apnea may be a risk factor for coronary artery disease.
People with sleep apnea are more likely to have coronary artery disease than those without sleep apnea. Additionally, sleep apnea may worsen existing coronary artery disease.
People with sleep apnea who underwent coronary bypass surgery had a higher rate of complications than those without sleep apnea.
Sleep apnea treatment may help reduce the risk of developing or worsening coronary artery disease.
Can Sleep Apnea Affect Your Heart?
Sleep apnea is a serious sleep disorder that occurs when a person’s breathing is interrupted during sleep. Although it can happen to anyone, it is more common in people who are overweight, have large tonsils, or have certain medical conditions.
Sleep apnea can cause various health problems, including heart disease. When someone has sleep apnea, their body doesn’t get the oxygen it needs. It can cause high blood pressure and other cardiovascular problems. In addition, sleep apnea can lead to oxidative stress, which is a type of damage to cells that can contribute to heart disease.
Do Heart Stents Qualify for VA Disability Benefits?
Several conditions may qualify for disability compensation, including heart disease. You may be eligible for benefits if you have a service-related heart condition requiring treatment with a stent.
To receive benefits, you will need to file a claim and get service-connected for it. It’s important to have your condition documented by a medical professional. You would need a diagnosis and a medical nexus letter that will link your condition to your service or service-connected disability.
Once your condition has been approved, you will be able to receive compensation based on the severity of your disability.
How Does Chronic Congestive Heart Failure Affect Ischemic Heart Disease?
Congestive heart failure is a common complication of ischemic heart disease. Veterans with Ischemic Heart Disease are nearly three times as likely to develop congestive heart failure as those without.
Congestive heart failure occurs when the heart cannot pump blood efficiently, causing a buildup of fluid in the lungs and other tissues. Symptoms of Congestive heart failure include shortness of breath, fatigue, and swelling in the legs and feet. If left untreated, it can lead to serious complications, including heart rhythm disorders, lung damage, and kidney failure.
There are two types of congestive heart failure:
Right-sided CHF: Right-sided CHF develops when the right ventricle struggles to deliver blood to the lungs. As blood backs up into the blood vessels, the body starts to retain fluid in the abdomen and lower body.
Left-sided CHF: Left-sided CHF is the most common form of CHF and begins when the left ventricle can’t effectively deliver blood throughout the body. Eventually, this can lead to fluid retention throughout the body (particularly around the lungs).*
*Cases of left-sided CHF can be further classified into one of two sub-types, characterized by the manner in which the ventricle is affected:
- Systolic CHF: Systolic CHF occurs when the left ventricle is unable to contract with enough force to circulate blood properly.
- Diastolic CHF: Diastolic CHF occurs when the heart muscle becomes stiff. Because the chamber must relax in order to fill with blood between contractions, this stiffness means that an inadequate amount of blood is available to pump to the rest of the body.
This guide is intended to provide an overview of the most common conditions secondary to ischemic heart disease. If you’re a veteran with ischemic heart disease and struggling to get the rating you deserve, the expert coaches at VA Claims Insider can help you file for a VA rating. We’ll help you gather the evidence and documentation you need to have the best chance of winning your claim. Contact us today to learn more about how we can help.
NEED MORE ASSISTANCE?
Most veterans are underrated for their disabilities and therefore not getting the compensation they’re due. At VA Claims Insider, we help you understand and take control of the claims process so you can get the rating and compensation you’re owed by law.
Our process takes the guesswork out of filing a VA disability claim and supports you every step of the way in building a fully developed claim (FDC). If you’ve filed your VA disability claim and have been denied or have received a low rating—or you’re unsure how to get started—reach out to us! Take advantage of a VA Claim Discovery Call. Learn what you’ve been missing—so you can FINALLY get the disability rating and compensation you deserve!
About the Author

Trisha Penrod
Trisha Penrod is a former active-duty Air Force officer. As an Intelligence Officer, she led teams of analysts to apply advanced analytic skills to identify, assess, and report potential threats to U.S. forces.
Trisha attended the U.S. Air Force Academy and holds an MBA from Webster University. After receiving an honorable discharge in 2018, Trisha worked as a growth marketer and utilizes her analytic skills to help others accomplish their business goals.



