Looking for Expert-Level VA Claim Answers?📱Call Us Now! 737-295-2226
Veterans are disproportionately at risk for cognitive disorders such as Alzheimer’s disease and dementia.
In this article, we’ll examine the different risk factors and explain how to prove service connection for a VA disability rating for Alzheimer’s (or other forms of dementia).
Veterans can qualify for up to a 100% VA disability rating for Alzheimer’s or other cognitive disorders.
Find out more about ratings with our Mental Health Ratings Guide and VA Ratings Guide.
Summary of Key Points
- Veterans face a higher risk for Alzheimer’s disease and other forms of dementia due to TBI, PTSD, chemical exposure, vascular conditions, and chronic sleep disruption.
- The VA rates Alzheimer’s and dementia at 0%, 10%, 30%, 50%, 70%, or 100%, depending on symptom severity and functional impairment.
- Service connection can be established directly or secondarily with a diagnosis, a strong nexus letter, and supportive statements from family or friends.
- Dementia can qualify for up to a 100% VA disability rating when symptoms severely limit daily functioning, communication, judgment, or independence.
Table of Contents
Deserve a Higher VA Rating?
Book a no-obligation VA Claim Discovery Call with an experienced team member. We’ll review your situation, spot what the VA may have missed, and help you map out a strategy to unlock the VA disability rating and tax-free compensation you’ve earned for your service. Click the red button below to book your call.
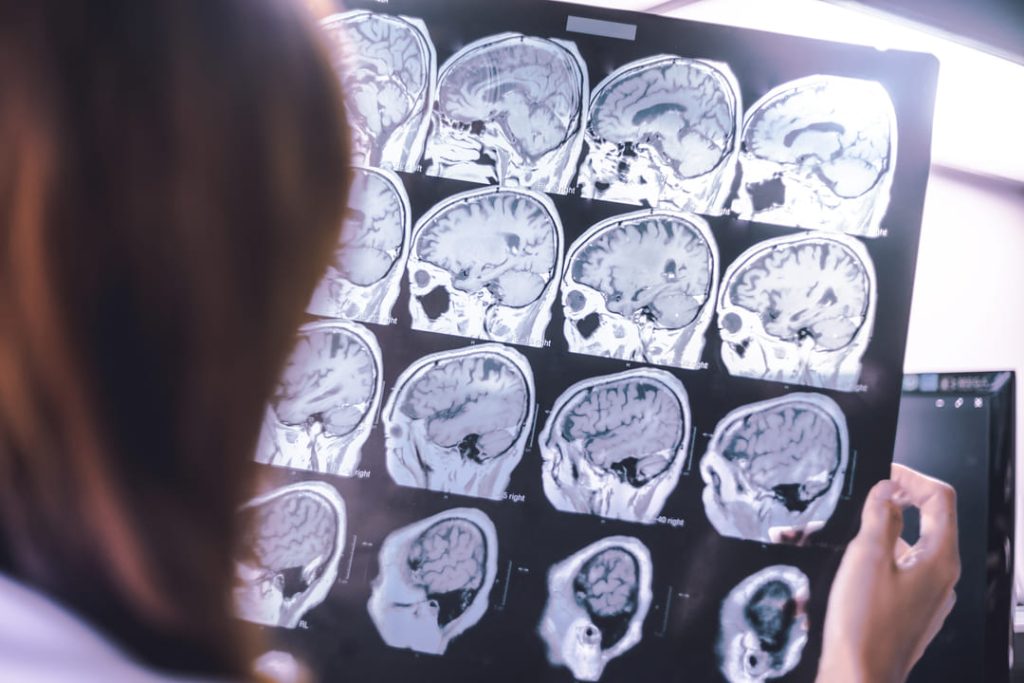
Getting a VA Disability Rating for Alzheimer’s (or Other Forms of Dementia)
A VA disability rating for Alzheimer’s (or other cognitive disorders) can be 0%, 10%, 30%, 50%, 70%, or 100%.
That means veterans can qualify for a VA disability rating for Alzheimer’s of up to 100%, based on severity of symptoms.
Proving Service Connection
As long as you can prove a service connection, it is possible to get up to a 100 percent VA disability rating for Alzheimer’s or dementia, depending on your symptoms. To get a VA rating for dementia (including an Alzheimer’s VA rating), begin with these steps:
Get a diagnosis.
- The first step in getting VA benefits for any cognitive disorder is to get an official diagnosis from a doctor (either VA or private). Your doctor will be looking for symptoms of different dementia disorders, including:
- Alzheimer’s disease: As the most common type of dementia, Alzheimer’s is characterized by plaques (clumps) or fibrous tangles of protein that build up in the brain. These plaques and tangles compromise healthy neurons and the fibers that connect them.
- Lewy body dementia: Like Alzheimer’s, this disease is also caused by “clumps” of protein. The proteins are balloon-like in shape and may also contribute to Parkinson’s disease. Though not as common as Alzheimer’s, Lewy body is still one of the most prevalent types of dementia. Symptoms include acting out dreams when sleeping, hallucinating, being unable to focus, losing coordination, having tremors, and physical rigidity (parkinsonism).
- Vascular dementia: This type of dementia occurs when the blood vessels that feed the brain become damaged. Symptoms center less on memory loss and more on declining problem-solving, thinking, and organizing abilities.
- Frontotemporal dementia: This is the rarest type of dementia and is marked by the breakdown of nerve cells—and connections between nerve cells—in the frontal and temporal lobes of the brain. It’s common for people with this type of dementia to experience a change in personality, behavior, judgment, and ability to communicate through language.
- Mixed dementia: It’s common for aging people to have multiple forms of dementia. If you have two or more types of dementia, it is considered mixed.
There’s no single test to determine if you have dementia. Instead, your doctor will examine your symptoms and history and conduct medical exams if needed to support or better define evidence of cognitive decline.
At your visit, your doctor may perform a series of physical tests to rule out other conditions. They will ask about your medical history and may have you take different cognitive or memory tests. They may also ask questions of your family members to learn about any changes in your cognitive and functional abilities.
In some cases, they may order cerebrospinal fluid tests to determine the ratio of proteins in the fluid (high quantities of protein may indicate certain types of dementia). They may also request a brain imaging test, such as an MRI, CT, or PET scan.
None of these tests is a one-and-done dementia detector, but they can help differentiate between different types of dementia. They can also establish a baseline to measure further cognitive decline.
The most important thing is that you see your doctor right away. Not only is this helpful for kickstarting your VA disability claim, but it can also benefit your cognitive function. Doctors can prescribe drugs and offer non-drug interventions to help you manage your symptoms. Some treatments may even be able to slow your cognitive decline.
Secure a nexus.
The easiest way to secure a nexus is often by way of a nexus letter. This evidence-based letter from a physician states that your dementia is likely service-connected. For example, the doctor may say that it is “more likely than not” that your dementia was caused due to your time in service. Click here to learn how to get a high-quality nexus letter at a reduced rate.
Solicit buddy letters or support statements.
In the case of dementia, letters from family, friends, and employers showing a decline in your cognitive abilities over time can be beneficial.

Dementia as a Secondary Condition
You can file a VA claim for dementia as a direct service-connected disability, which means it developed as a direct consequence of your military service. You can also file for dementia as a secondary service-connected disability, which means that it developed or grew worse due to another condition. One example would be filing for dementia secondary to hearing loss.
A direct or secondary service connection can qualify you for a VA rating for Alzheimer’s or dementia. The main thing is that you get your dementia service-connected.
If you or someone you love has dementia caused or worsened by military service, you shouldn’t suffer without help.
Contact us for resources to help you file for 100 percent VA disability benefits and learn about other VA benefits that may be available to you. These may include memory care, assisted living or nursing home care, home-based care, and respite care for caregivers.
What’s the Difference Between Dementia and Alzheimer’s Disease?
These conditions are often referred to interchangeably, but they are different. Dementia is a general term that refers to a declining ability to remember, think, focus, reason, make decisions, or communicate.
While dementia is an umbrella term, Alzheimer’s disease is one specific type of dementia—the most common type.
In its early stages, Alzheimer’s symptoms may include:
- A decline in memory that disrupts daily life
- Forgetting where you are, getting lost
- Misplacing things
- Forgetting information that you just learned
- Poor judgment/decision-making abilities
- Loss of sense of initiative
- Loss of interest in things that you usually enjoy
- Taking longer to accomplish daily tasks
- Difficulty solving problems
- Changes to mood and personality (including becoming more aggressive)
- Elevated anxiety
Moderate to severe symptoms may include:
- Increased sense of confusion
- Self-isolating
- Difficulty communicating through language
- Difficulty transitioning to new situations
- Inability to recognize family and friends
- Hallucinations, paranoia, delusions
- Inappropriate behavior and outbursts
- Sadness, restlessness
- Groaning, moaning, or grunting,
- Increased sleep
- Loss of bowel and bladder control
- Seizures

Why are Veterans at a Greater Risk for Dementia?
Data from the Centers for Disease Control (CDC) shows that 1 in 9 veterans aged 45 years and older have subjective cognitive decline. The average age of a veteran today is 58 years old. Since most cases of late-onset Alzheimer’s (the most common type of dementia) develop among people in their mid-60s, it’s clear that many more veterans could be facing this disease in the near future.
Let’s look at the unique risk factors that could increase veterans’ risk for dementia, including Alzheimer’s.
Traumatic Brain Injury (TBI)
Veterans’ combat injuries, including blast exposure, make them vulnerable to TBIs. In fact, research shows that up to 28% of service members experience a TBI. Unfortunately, TBIs can lead to other long-term problems, including cognitive decline. Numerous studies have established a link between moderate-to-severe TBIs and an elevated risk of developing certain types of dementia later in life.
For example, a 2018 JAMA Neurology study compared dementia diagnoses in veterans who had developed traumatic brain injuries (with or without loss of consciousness) and those without TBI exposure. The study found that 2.6 percent of veterans without TBI developed dementia compared to 6.1 percent of those who had experienced TBI.
The study also showed that those who had experienced even mild TBI without loss of consciousness had more than twice the risk of dementia.
PTSD and Major Depressive Disorder
Post-traumatic stress disorder (PTSD) and major depressive disorder (MDD), which are both common in veterans, are associated with double the risk of developing dementia or cognitive impairment at age 56 or older.
Peripheral Arterial Disease
Peripheral arterial disease (PAD) is a buildup of plaque (from fat and cholesterol) in the legs and arms. PAD makes it harder for your blood to carry nutrients to your limbs.
Recent research shows that PAD disproportionately affects veterans and that many aren’t getting sufficient care.
It’s well-known that PAD puts veterans at greater risk for adverse health outcomes such as heart attack and stroke, but recent studies have shown a link between PAD and cognitive impairment.
Chemical Exposure
Military service can expose members to all kinds of chemicals. Among the many harmful effects of this exposure is a heightened risk for dementia. One 2021 JAMA Neurology study of 300,000 Vietnam-era U.S. veterans showed that those exposed to Agent Orange were two times as likely to develop dementia and to develop it at an earlier age as those who weren’t exposed.
Another source of chemical exposure for veterans is jet fuel. Jet fuel is filled with many known carcinogens and toxins. These chemicals are associated with significant health risks, including cancer, sleep apnea, asthma, and Parkinson’s disease. The chemicals have also been linked to cognitive decline for those with relatively high exposure, including failing focus, memory, and executive function.
Sleeplessness and Insomnia
Research correlates insomnia with cognitive decline. Sleep is a key factor in learning and memory consolidation. If you don’t get enough sleep, you’re at a higher risk for developing Alzheimer’s disease.
Unfortunately, insomnia is a common problem in the military. A 2021 DOD report to Congress revealed that 55% to 76% of military members do not get the recommended seven hours of sleep compared to 28% to 37% of the overall U.S. population that falls below this threshold.
There are a number of reasons troops aren’t getting all the sleep they need. They include rigorous deployment schedules, frequent changing of time zones that disrupt circadian rhythms, lack of sunlight due to shift work or work in high-security SCIFS (sensitive compartmented information facility), and a high incidence of PTSD, which can disrupt sleep patterns.
RELATED: VA Disability for Memory Loss
NEED MORE ASSISTANCE?
Most veterans are underrated for their disabilities and, therefore, not getting their due compensation. At VA Claims Insider, we educate and support you to understand and take control of the claims process, so you can get the rating and compensation you’re owed by law.
Our process takes the guesswork out of filing a VA disability claim and supports you every step of the way in building a fully-developed claim (FDC)! If you’ve filed your VA disability claim and have been denied or have received a low rating—or you’re unsure how to get started—reach out to us! Take advantage of a VA Claim Discovery Call. Learn what you’ve been missing—so you can FINALLY get the disability rating and compensation YOU DESERVE!
FAQs | Frequently Asked Questions
Is Alzheimer’s disease considered a VA disability?
Yes. Alzheimer’s and other forms of dementia are ratable VA disabilities when you can prove service connection.
What is the VA rating for Alzheimer’s or dementia?
VA ratings range from 0% to 100% under the General Rating Formula for Mental Disorders. Veterans with severe cognitive decline or inability to function independently may qualify for 100%.
How do I prove my dementia is service-connected?
You’ll need a diagnosis, a medical nexus linking your condition to service, and supporting evidence such as buddy statements or documentation of risk factors (TBI, PTSD, exposure, etc.).
Can dementia be claimed as a secondary condition?
Yes. Dementia can be secondary to conditions like hearing loss, PTSD, vascular disease, sleep apnea, or other service-connected disabilities that contribute to cognitive decline.
Are veterans at higher risk of developing dementia?
Yes. Studies show elevated rates connected to TBIs, PTSD, chemical exposures (like Agent Orange or jet fuel), vascular disease, and chronic sleep disruption.
About the Author

Clay Huston
Clay Huston is a former U.S. Army Reserves Blackhawk Pilot and officer. Clay enlisted in the Army in 2013 and was commissioned as a 2LT in 2017 after earning a business degree from the University of Illinois Champaign-Urbana.
Since separating from the military, Clay has pursued a career as a writer. He also runs the nonprofit notfatherless.org, which fundraises for Children’s Homes in Mexico.



